Submitted by obuadmin on
The challenge of making an acute clinical decision about transfusion is to assess the likely benefts for the individual patient (PMID 12076437). One way to aid clinical decision-making is to use a simple checklist (downloadable from end of page>) such as the following to help focus the decision):
- What improvement in the patient’s clinical condition am I aiming to achieve?
- Can it be achieved without transfusing?
- Can I minimize blood loss to avoid the need for transfusion?
- Are there any other treatments I should give before making the decision to transfuse (such as intravenous replacement fuids oxygen, inotropes)?
- What are the specifc clinical or laboratory indications for transfusion for this patient at this time?
- What are the risks of infection or some other severe adverse event?
- Do the benefts of transfusion outweigh the risks for this particular patient?
- Will a trained person respond immediately if an acute transfusion reaction occurs?
- If this blood was for my child, or myself would I accept the transfusion or not?
- Have I recorded on the patient’s chart (and signed) my decision and my reasons for transfusion?
Decision-making can be relatively straightforward when a patient has a life-threatening major haemorrhage, bleeding associated with profound thrombocytopenia, or severe, disabling symptoms of anaemia associated with cancer chemotherapy. Indications for transfusion may also be clear in conditions such as thallasaemia or myelodysplastic disease. The decision can be much less clear – for example in an elderly patient, who has a haemoglobin concentration of 80g/l, has no evident symptoms of anaemia, is haemodynamically stable and is not bleeding.
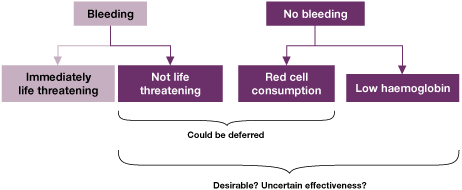
Figure 7.2 What makes us transfuse red cells
| Attachment | Size |
|---|---|
| 51.08 KB |
